Jennifer from Austin sent us this question:” I have severe pain and difficulty swallowing after hiatal hernia repair and LINX™ surgery.
I would like to ask if you can describe the surgery that I need to have to fix this problem and what kind of surgeon can take care of it. Please and thank you so much.”
Dear Jennifer,
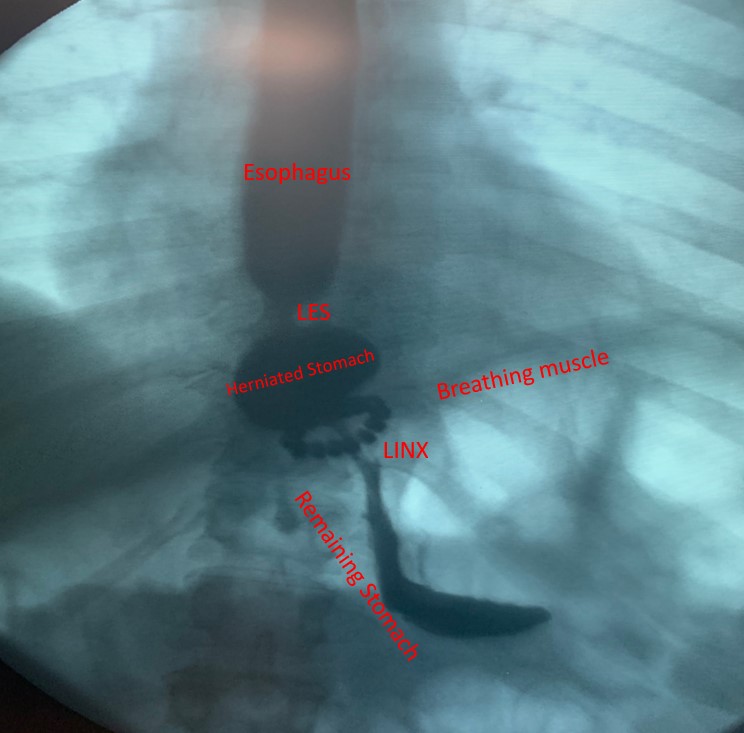
Contrast study and upper endoscopy pictures show a recurrent hiatal hernia with part of the stomach slipping through LINX™ device into chest. The LINX™ device is just below the diaphragm or breathing muscle. If the hiatal hernia recurrence occurred several months after initial surgery, the magnetic ring now tightly adherent to esophagus due to scar tissue formation, would have mostly likely migrated into chest along with the esophagus. Proximal stomach will remain in this case below the level of the LINX™ device.
 The primary cause for hiatal hernia recurrence is poor esophageal mobilization. During hiatal hernia repair, lower esophagus and herniated stomach are completely freed from all surrounding scar tissue caused by hiatal hernia. This step is crucial to drop the lower esophagus and stomach back into original position below the breathing muscle. Once this step is accomplished, hiatal hernia repair is completed by closing the hiatal opening with sutures. A bioabsorbable mesh is sometimes used to reinforce the repair.
The primary cause for hiatal hernia recurrence is poor esophageal mobilization. During hiatal hernia repair, lower esophagus and herniated stomach are completely freed from all surrounding scar tissue caused by hiatal hernia. This step is crucial to drop the lower esophagus and stomach back into original position below the breathing muscle. Once this step is accomplished, hiatal hernia repair is completed by closing the hiatal opening with sutures. A bioabsorbable mesh is sometimes used to reinforce the repair.
Additional risk factors for recurrent hiatal hernia include shortened esophagus, advanced patient age and severe coughing and/or dry heaving immediately after surgery. Patients typically develop dysphagia (difficulty swallowing), chest pain and recurrent acid reflux symptoms like heartburn and food regurgitation. I recommend evaluation by a competent acid reflux specialist followed by surgical exploration, reduction of hiatus hernia and LINX™ device, proper esophagus mobilization, and closure of hiatal opening with mesh reinforcement.